Mask Off: How COVID-19 Exposed Racial Disparities in Healthcare
The COVID-19 pandemic has laid bare the ways in which historical injustices have perpetuated inequities in quality healthcare access for communities of color.
By: Vineet Singal, CEO & Co-Founder of CareMessage
“Of all the forms of inequality, injustice in health is the most shocking and inhumane.”
— Dr. Martin Luther King, Jr.
Introduction
Agustín Rodríguez was a quiet, deeply religious man originally from El Salvador. He worked in a pork processing plant in Sioux Falls, South Dakota, where he had a rough job sawing the legs off of dead pigs. He spent most of his time with his wife, Angelita, whom he married a month after they met more than 24 years ago.
In early April, Angelita noticed that the lunch she had packed for her husband had come back uneaten. Then came the fever, the aches, the chills, the shortness of breath. He mopped floors with a fever shortly before he was hospitalized. By April 14, Agustín died, a victim of COVID-19.
Angelita later mentioned to a news source: “I took him to the hospital and left with nothing. Now I have nothing.” The 73-year-old widow also shared that she has now developed a cough.
The pork processing plant where Agustín worked is owned by a company, Smithfield, which is one of the largest pork producers in the world. Despite identifying the first COVID-19 case at the plant on March 24, the plant did not officially close more than 20 days later until April 15, when ~800 of its workers had been diagnosed with COVID-19, making it one of the largest hotspots for the coronavirus outbreak nationally.
BBC News reported that, “according to Smithfield employees, their union representatives, and advocates for the immigrant community in Sioux Falls, the outbreak that led to the plant closure was avoidable. They allege early requests for personal protective equipment were ignored, that sick workers were incentivised to continue working, and that information regarding the spread of the virus was kept from them, even when they were at risk of exposing family and the broader public.”
In addition, according to the CDC,
While more than 40 languages are spoken at the plant, workers were sent home with informational packets that were written only in English.
The CDC concluded that this lack of communication was part of the reason why so many people did not have the necessary information to prevent the spread of COVID-19 at the workplace.
Agustín’s story is personally meaningful to me because my parents live within a 10-minute drive of this pork processing plant where Agustín and so many others needlessly acquired COVID-19. My mother is the only anesthesiologist at her hospital and is in charge of ventilators. My father, a transplant hepatologist, is seeing patients that are at the highest risk of COVID-19 complications given underlying GI and liver conditions. In addition to the risk to its employees and their families, Smithfield’s actions have put at risk the lives of thousands of frontline health workers, including those of my parents.

An early photo of me and my parents
But this story has been eating at me for another reason. Growing up in multiple, mostly homogenous countries, my family and I experienced discrimination and violence because of the color of our skin and the religion we practiced. All things considered though, I have lived a very privileged life as a straight, educated son of two doctors. Serving as the CEO and Co-Founder of CareMessage has required me to step outside of my comfort zone, first through my volunteer work at free medical clinics and then subsequently through witnessing the on-the-ground challenges directly through our clinic partners.
Perhaps one of the most helpful and educational experiences for me has been the many conversations I’ve had with members of my team, many of whom come from backgrounds similar to our patients. Those conversations have provided me with an appreciation for not only the historical context behind the current realities for our patient populations, but also a visceral perspective on these issues that is invaluable to understand them fully.
This pandemic, in many ways, has exposed much of what we already know to be true about the unfortunate state of healthcare disparities in this country, and the output of that is playing out in the worst possible way. At CareMessage, we have spent more than seven years tackling disparities that have led to disproportionate access to healthcare and outcomes for underserved populations, particularly communities of color. While we’ve made significant progress in helping narrow the gap, the COVID-19 pandemic’s impact on communities of color illustrates how much work still needs to be done.
In this post, I hope to outline some of what I’ve learned in the past few weeks on COVID-19 related disparities for communities of color, while also sharing some learnings into the historical inequities that have led to the disparities we’re seeing today.
My hope is that readers walk away with a more holistic understanding of these issues, and work within their communities to drive change. We need multi-faceted support — from government, philanthropy, healthcare providers, community organizations — in order to directly address these issues. In that vein, I also hope to outline what CareMessage is doing to help, and what others can do to support our efforts.
The Data
Black populations: According to the American Public Media (APM) Research Lab, which compiled data from the 35 states (and the District of Columbia) that are now reporting racial demographics for COVID-19 deaths, as of April 30, black Americans are dying at 2.6 times the rate of whites. As of April 30, black Americans are dying at 2.6 times the rate of whites.
According to the APM Research Lab, “in some places, the multiple between black and white mortality rates greatly exceeds the 2.6 overall figure that we’ve constructed from all available data for the nation. In Kansas and Wisconsin, black residents are 7 times more likely to die than white residents. In Washington D.C., the rate among blacks is 6 times higher than whites, while in Michigan and Missouri, it is 5 times greater. In Arkansas, Illinois, Louisiana, New York State, Oregon, and South Carolina, blacks are 3–4 times more likely to die of the virus than whites.”
Latinx and Native American populations: For the Latinx and Native American patient populations, while the overall national disparities in terms of morbidity are not as significant as for the black patient population, significant disparities still exist in major metropolitan areas (for Latinx populations) and rural areas (for Native American populations).
In New York, Latinos are dying at a higher rate than any other group, making up 26% of deaths. The trend is comparable across the country in the SF Bay Area. In San Francisco, Latinos account for 15% of the population but comprise 25% of confirmed COVID-19 cases. In Santa Clara County, Latinos account for 26% of the population, and 36% of confirmed cases. According to the Illinois Department of Public Health, 30% of the state’s COVID-19 patients are Latino/Hispanic, while only accounting for 17% of the overall population.
New statewide data shows that more than 20% of all positive cases in New Mexico are Native Americans, while only making up only 5% of New Mexico’s population. The Navajo Nation, the largest Indigenous reservation in the country with a land area bigger than 10 US states, has been ravaged by the COVID-19 epidemic. The Nation stands only behind New York and New Jersey in the total number of COVID-19 cases per capita. The Navajo Nation, the largest Indigenous reservation in the country with a land area bigger than 10 US states, has been ravaged by the COVID-19 epidemic.

Korene Atene, a nursing assistant, gets information from people lined up to get tested for COVID-19 in Oljato-Monument Valley, Navajo Nation. Kristin Murphy/The Deseret News/AP
Dr. Utibe R. Essien et al. summarize these findings in a sobering JAMA article: “The burden of COVID-19 morbidity and mortality has disproportionately fallen on minority populations. Early in the pandemic, lower rates of COVID-19 testing were reported among minority communities. Now, emerging data illustrate that black and Hispanic Americans are dying at far higher rates from the novel coronavirus than any other group in the nation. These disparities are just the most recent manifestation of centuries’ worth of racial and ethnic gaps in health outcomes.”
Historical Injustices and Inequities
“An America that asks what it owes its most vulnerable citizens is improved and humane. An America that looks away is ignoring not just the sins of the past but the sins of the present and the certain sins of the future.”
— Ta-Nehisi Coates
On April 10, US Surgeon General Jerome Adams said that black, Latino, and other people of color should “avoid alcohol, tobacco, and drugs” and need “to step up” in order to curb the growing COVID-19 rates within these populations. The Surgeon General received criticism for his victim-blaming remarks, and his comments also reignited important conversations around the historical inequities that have put us in this position.
In his New York Times column on COVID-19 disparities, Jamelle Bouie described the historical inequities that have originated from this country’s original sin, slavery:
“The Civil War may have destroyed slave society, but the racial hierarchy that was central to that society survived the carnage and disruption of the conflict to shape the aftermath, especially in the absence of a sustained program to radically restructure the social and economic life of the South.”
He continues by describing how the inequities continued into the 20th century, with the rapid industrialization of the country that relegated blacks to low wage positions and New Deal stimulus efforts that explicitly promoted the interest of whites.

Industrialization of America, Photo by: Elina Krima / Pexels
All of this happened in the backdrop of structural racism that made life stressful and unequal. Bouie explained:
“It’s not that life was particularly good for white workers, but that blacks faced additional challenges, from the denial of formal political rights to social exclusion and widespread, state-sanctioned violence. If they lived in cities, blacks were relegated to the least sanitary neighborhoods with the most substandard housing; if they had a skill or knew a craft, they were excluded from the guilds and unions that would have given them a path to employment; if they possessed a formal education, they were barred from most middle-class professions.”
Ta-Nehisi Coates articulated the connection between historical injustices and current disparities in his landmark 2014 essay titled The Case for Reparations, where he stated “All of our solutions to the great problems of health care, education, housing, and economic inequality are troubled by what must go unspoken”, referring to the historical injustices afflicted on communities of color. The downstream effects of these historical inequities have persisted to this day, leading to disparities that directly impact people’s health.
High rates of asthma amongst black children can be traced back to redlining laws instituted 80 years during the New Deal era. Dr. Neera Thakur, an assistant professor at UCSF who oversaw a 2019 study on the impact of redlining, concluded that “even though a policy gets eliminated or is recognized to be a poor choice, its effect can have impacts even many decades later.”
Healthcare disparities facing Native American communities have compounded over centuries of neglect and underfunding. According to Dr. David Marshall, a public health professor at Harvard, “if you look at every program that provides health care, the per capita funding is lowest [sic] for the Indian Health Service than it is for Medicaid, the VA, any other program in the United States — it receives the lowest per-person funding.” It is therefore no surprise that Native American populations are 200 times more likely to die of diabetes than any other group, and more than 25% lack basic health insurance.
Bouie summarizes the impact of these inequities thusly: “Race…still answers the question of ‘who.’ Who will live in crowded, segregated neighborhoods? Who will be exposed to lead-poisoned pipes and toxic waste? Who will live with polluted air and suffer disproportionately from maladies like asthma and heart disease? And when disease comes, who will be the first to succumb in large numbers?”

A bus full of bags of food, fruit, and milk for the needy and homeless pulls up to the Pope Francis Center in Detroit on April 9. Eric Seals, Detroit Free Press.
These historical injustices resulted in two major downstream effects that had a direct impact on people’s health: (A) Discrimination and Unconscious Bias in Healthcare and (B) Poverty and Lack of Access to Essential Needs.
Discrimination and Unconscious Bias in Healthcare
“The legacy of the study at Tuskegee has reached far and deep, in ways that hurt our progress and divide our nation. We cannot be one America when a whole segment of our nation has no trust in America.”
— Bill Clinton
The topic of healthcare is a sensitive one for communities of color given fairly recent discriminatory actions against them. The most notorious example is the Tuskegee study, where poor and illiterate (and mostly black) sharecroppers were enrolled in a study of syphilis, and hundreds were not given penicillin when it was found to be a cure. Many died, and many more were infected.
Essien at al. share that these incidents have created an enduring mistrust of the healthcare system, from the point of view of immigrant populations: “The fear of potential rationing of critical care resources has heightened in communities of color for whom long-standing discrimination and mistrust of the health care system have persisted. Undocumented immigrants have lower rates of health insurance coverage and an added fear of deportation.”
This mistrust is further exacerbated by documented, proven bias and discrimination in our healthcare system towards people of color. According to a 2017 meta-analysis (a review of 42 studies) published in BMC Ethics, the researchers concluded that [‘physicians’] biases are consistent with those of the general population” and cautioned that “these biases are likely to affect diagnosis and care.” The Washington Post has reported, “in treatment of other maladies, including osteoarthritis, cardiovascular disease, and cancer, white physicians harbor implicit preferences for white patients over black ones.” Moreover, an October 2015 report published by the American Medical Association showed that “on average, white Americans spent 80 minutes waiting for or receiving care, while black Americans spent 99 minutes and Latinos 105 minutes waiting for that same care.”
Implicit, or unconscious, bias seems to be the main culprit here. Dr. Aaron Cornell, a professor at the Indiana University School of Medicine, summarized the manifestations of implicit bias research in a New York Times Op-Ed: “Physicians sometimes had a harder time making accurate diagnoses because they seemed to be worse at reading the signals from minority patients, perhaps because of cultural or language barriers. Then there were beliefs that physicians already held about the behavior of minorities. You could call these stereotypes, like believing that minority patients wouldn’t comply with recommended changes.”
These biases have continued in the COVID-19 era. NPR reported that a big data firm that reviewed recent billing information in several states found that a black patient with symptoms like cough and fever was less likely to be given one of the scarce coronavirus tests. And perhaps one of the most disturbing stories is that of Gary Fowler, who died at the age of 56 in Detroit from COVID-19 related complications.

The Gambrell-Fowler family pose for a family portrait. From left are Keith Gambrell, Gary Fowler, Cheryl Fowler, Troy Fowler and Paris Fowler. (Photo: Billy Edwards)
Mr. Fowler, a black man, went to three metro-area Detroit hospitals begging for a COVID-19 test but was turned away each time despite demonstrating all the telltale signs of the infection.
Mr. Fowler’s stepson, Keith, described the dilemma that so many people like his father face: “I honestly think that’s why the death rate for blacks is so high. It’s because we’re being pushed to the back and told to go home, but come back if you can make it before you die.”
Poverty and Lack of Access to Essential Needs
“Why is it that farmworkers feed the nation but they can’t get food stamps?”
— Dolores Huerta
Compounding the impact of implicit bias and discrimination are the daily struggles of poverty, including access to essential needs such as food, housing, clean air, clean water, employment, and others. The current crisis has exposed the ever-widening income inequality in the United States that has had a direct impact on people’s health. In fact, a recent JAMA study conducted by UCLA researchers evaluated health data collected by the CDC from 1993 to 2017. The researchers concluded that of all the factors they evaluated, including gender, race, and age, “income was the biggest predictor of differences in health outcomes” and that in the last 25 years, “health differences between the highest income group and lowest income group [have] increased.”
COVID-19, however, is making an already terrible health situation significantly worse, especially for low-income communities of color. A major driver of this is the employment sectors these populations tend to occupy, including retail clerks, grocery and restaurant service workers, public transportation drivers, home health aides, hospital cleaning staff, etc. that are considered “essential services” during the pandemic. Compounding these issues is the lack of personal protective equipment (PPE) that has been afforded to these essential staff, creating a vicious cycle of infection within these communities. The fear of losing one’s job — echoed by employees at the Smithfield pork plant in South Dakota and so many others nationwide — ensures that these workers are forced to come to work, even if they might be at high risk of contracting the virus and/or developing complications as a result.
Amidst the broader population, rampant unemployment is only worsening the demand for essential needs within low-income communities of color. The Navajo Nation is struggling with challenges tied to a lack of running water, and one Navajo doctor in Arizona remarked,
“You’re saying 20 seconds of [washing] your hands with water. We do not have plumbing.”
While a number of organizations are focused on tackling resource challenges tied to food and water, there are other issues much harder to solve, including clean air. In an analysis of 3,080 counties in the United States, researchers at the Harvard School of Public Health found that higher rates of pollution were associated with higher death rates from COVID-19, with the American Lung Association expressing concern that the “findings were particularly important for hospitals in poor neighborhoods and communities of color, which tend to be exposed to higher levels of air pollution than affluent, white communities.” Another factor leading to increased rates of infection is the high rate of incarceration amongst low-income communities of color, especially black communities.
Finally, what is perhaps most concerning from a long-term recovery standpoint is the emotional toll that this pandemic is likely to take on communities of color, already exacerbated by the daily struggles of poverty and racial bias. In fact, merely being black in the United States is linked to premature biological aging, a phenomenon called the “weathering effect.” A licensed social worker who primarily provides therapy to black women in Connecticut reflected that her clients “are starting to feel hopeless and helpless.”
Manuel Castro, the executive director of New Immigrant Community Empowerment, recently shared how overwhelmed his organization has been with requests for food from undocumented New Yorkers who are either sick and/or out of work, and was planning to draw names out of a hat to decide which families would get the limited supplies the organization has on hand. Regarding this decision, he later remarked: “How do you do that? They’re asking for food. They’re asking for jobs. And we don’t have much to give.”
Our Response: CMLight and Project Equity
Our mission at CareMessage is to leverage technology to help safety-net organizations fulfill the essential needs of underserved populations. Since mid-March, our executive team and I have guided our teams to respond swiftly to the COVID-19 crisis. Over the past two months, CareMessage has facilitated ~10M COVID-19-specific messaging interactions with several million patients. The following map illustrates our reach nationally — each number represents the total number of messages sent per state as of May 11, 2020.
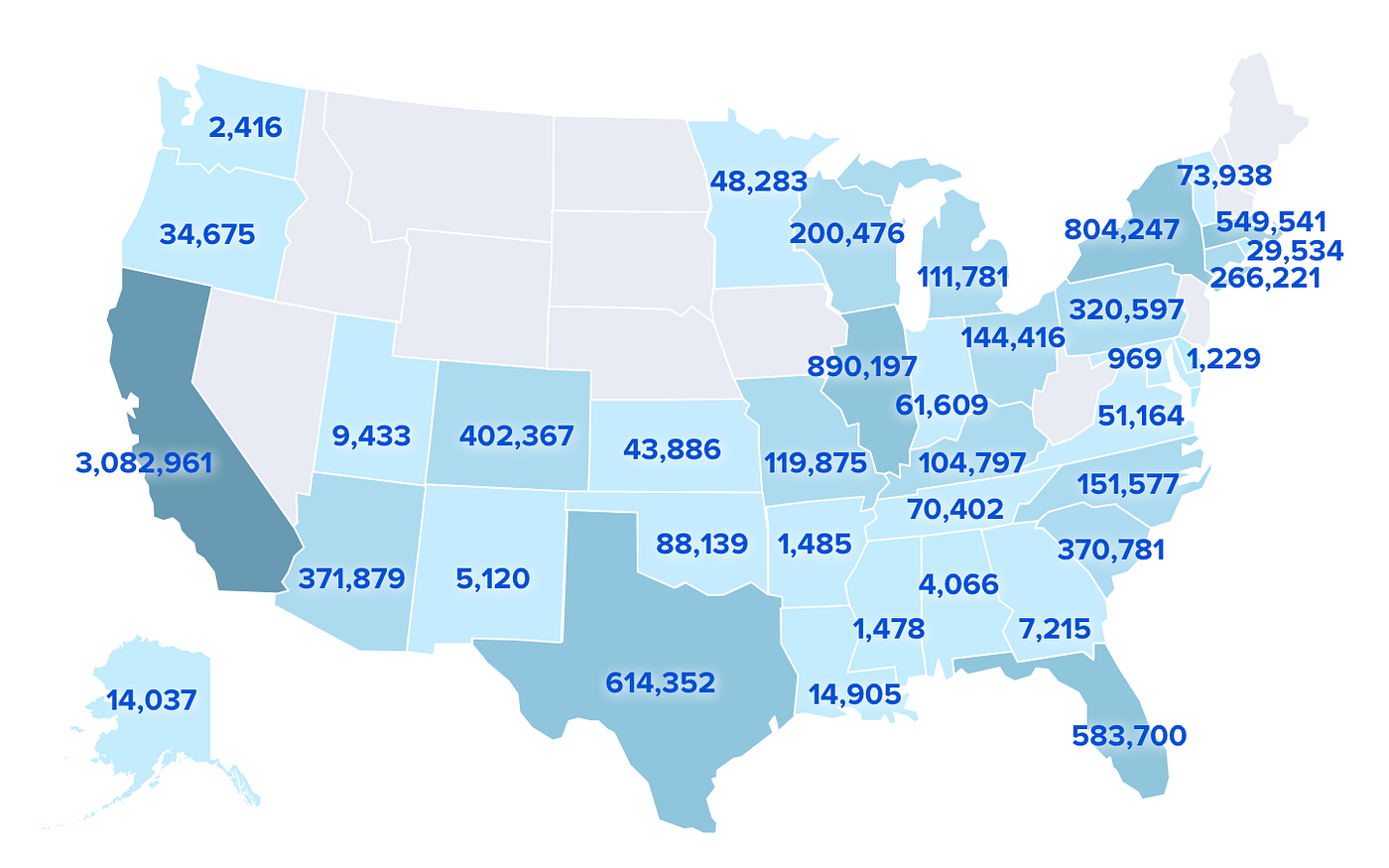
The number of COVID-19 messages sent by state through CareMessage as of May 11, 2020
We have seen first hand the power of technology in enabling safety-net provider networks nationally provide critical information to and collect data from their patients via texting, which has proven to be the most effective method of engaging low-income patients. Leveraging CareMessage, our partner clinics are accomplishing the following goals:
- Preventing Spread: Provide education around COVID-19 spread, including self-quarantine instructions and other preventive measures.
- Testing for High-Risk Groups: Coordinate drive-thru and rapid testing.
- Care Coordination: Coordinate care for patients via Telehealth, and provide the necessary education for first-time telehealth users
- Adherence to Chronic Disease Management: Support adherence to treatment/behavioral regimen for underlying chronic conditions to minimize the risk of complications in the event of a positive COVID-19 diagnosis.
- Connection to Resources: Support patients as they navigate basic needs such as healthy food, medication, and unemployment benefits by providing information on local resources.
- COVID-19 Treatment/Vaccination: Over time, we anticipate that the focus will shift toward ensuring COVID-19 patients are able to receive and adhere to treatment, and others are able to get vaccinated.
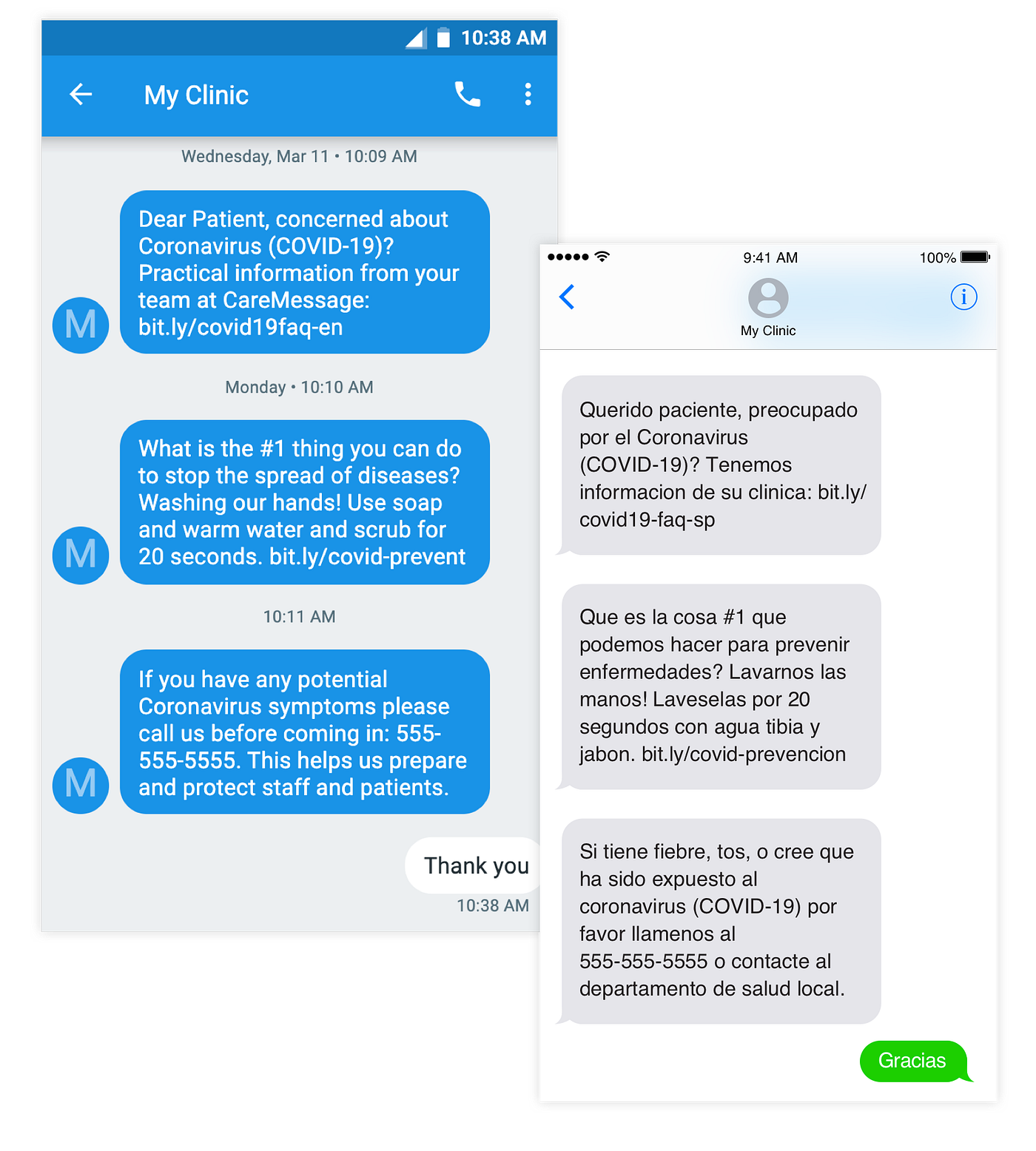
While we believed it was imperative to support our existing partners, we strongly felt we had to do more. On March 20th, we launched CMLight, a philanthropically-subsidized, COVID-19-specific messaging platform that made a COVID-19 version of our platform (messaging functionality alongside an entire library of COVID-19 messaging content) free for at least 60 days to any safety-net organization across the country. In the last few weeks, more than 100 safety net organizations serving nearly 1.5 million patients have adopted CMLight to reach their patients.
The black, Latinx, and Native American communities make up 31% of the US population, yet represent 60% of patients served at safety net providers, our primary focus. Through both our pre-COVID clinic partners and CMLight partners, we currently serve nearly three million black, Latino, and Native American patients through these safety net provider organizations. Furthermore, CareMessage’s messages are crafted at a sixth-grade reading level or below and are tailored for cultural relevance.
Recently, our team — with my encouragement and full support — launched Project Equity, an organizational initiative to further our commitment to addressing healthcare disparities in COVID-19. This is a more focused continuation of our existing efforts, and reflects the alarming realities on the ground that are impacting COVID-19 outcomes for communities of color. We are proud and honored that Johnson and Johnson and the Wagner Foundation have led the initial commitments to fund Project Equity, and we are looking forward to partnering with additional philanthropists and funders to continue to support these efforts. The effort encompasses the following two major initiatives:
- Targeted Dissemination of CMLight: We plan to disseminate CMLight in a more targeted way to extend our reach deeper into black, Latinx, and Native American communities nationwide. We plan to do so through targeted outreach to health centers and free clinics in cities and states with a high number of low-income black, Latinx, and Native American patients, alongside partnerships with national, state and local organizations and government agencies. To start, we are proud to partner with national agencies such as the National Association of Community Health Centers and the National Association of Free and Charitable Clinics.
- Webinar Series on Healthcare Disparities in COVID-19: We have launched a webinar series that focused on discussing COVID-19-related issues affecting low-income communities of color, with participation from leading experts on these issues that also come from these communities. The goal of these webinars is to provide a forum to provide both education as well as actionable guidance to healthcare providers on the frontlines as they develop policies and workflows to address healthcare disparities (including leveraging CareMessage/CMLight). We conducted the first webinar last week with more than 150 attendees representing more than 100 healthcare provider organizations nationally. The next webinar is scheduled for May 13 and will focus on disparities in Latinx communities. We plan to announce future webinars on our Twitter account.
Partner With Us
I want to acknowledge and thank our team, our healthcare clinic partners, our board, our donors, and our advisers and colleagues. This work would not be possible without your tireless efforts.
We remain committed to devoting major resources internally to these efforts, and invite others to join us as we continue to make progress.
- If you are a safety-net healthcare provider with a strong focus on black, Latinx and Native American populations, we invite you to apply for access to CMLight here.
- If you are a government agency, especially representing a city, county, state or tribe with a major COVID-19 response effort for communities of color, please feel free to contact us to explore how we may be able to work together.
- If you are a philanthropist or funder interested in supporting Project Equity, please feel free to contact me at vineet@caremessage.org.
As we look to the future, I think it’s only appropriate to end this post with this hopeful message from Dr. Essien and colleagues:
“This month marks the 105th anniversary of the establishment of Negro Health Week, an effort founded by Booker T. Washington and created to raise awareness about the health disparities that continue to affect racial minority communities today. Just 3 years after that inaugural event, the 1918 influenza pandemic was rampant across the US. We do not yet know the full course of the current COVID-19 pandemic, but if we can boldly address health equity in this crisis today, we have the opportunity to greatly shape how history looks back at this moment — and perhaps permanently reduce health disparities moving forward."
